Sound of a Breakthrough: Regeneron's Otarmeni Approval Marks the Dawn of Gene Therapy for Hearing Loss
On April 23, 2026, the FDA granted accelerated approval to Regeneron's Otarmeni, the first gene therapy ever approved for genetic hearing loss—a breakthrough that represents a categorical shift in what medicine can do.

There is a category of medical milestone that arrives not as an incremental improvement but as a categorical shift in what medicine can do. On April 23, 2026, the FDA granted accelerated approval to Regeneron's Otarmeni, the first gene therapy ever approved for genetic hearing loss. The drug, known chemically as lunsotogene parvec-cwha, targets a rare but devastating condition caused by variants in the OTOF gene, which encodes the otoferlin protein essential for transmitting sound signals from the inner ear to the brain. For the roughly 50 newborns affected in the United States each year, the approval represents something that did not exist before: a treatment that can restore the ability to hear.
What makes this approval remarkable is not just the science, though the science is genuinely extraordinary. It is the convergence of several forces that rarely align in pharmaceutical development: a compelling clinical result, a novel regulatory pathway, a pricing decision that defies industry convention, and a strategic signal from one of the sector's most scientifically credible companies about where genetic medicine is heading.
What Otarmeni Does and What the Data Show
Otoferlin sits at the base of the sensory hair cells in the cochlea and acts as the molecular linchpin that enables those cells to communicate with the auditory nerve. Without a functional otoferlin protein, the ear's mechanical structures are intact but the signal never reaches the brain. Children born with biallelic variants in the OTOF gene are profoundly deaf from birth, not because their ears are structurally damaged but because a single protein is missing from the chain of events that converts sound into perception.
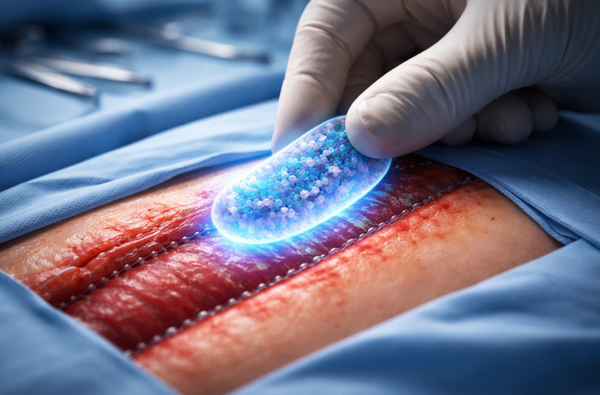
Otarmeni addresses this directly. It uses an adeno-associated virus vector to deliver a working copy of the OTOF gene into the cochlea via a surgical infusion similar to cochlear implantation. The newly introduced gene is placed under the control of a proprietary Myo15 promoter designed to restrict expression specifically to the hair cells that normally produce otoferlin. The approach is precise, targeted, and designed to be durable.
The pivotal CHORD trial enrolled 20 participants aged 10 months to 16 years, all with profound hearing loss at baseline. The results were striking. Eighty percent of participants achieved the primary endpoint, defined as hearing improvement to a threshold of 70 decibels or better at 24 weeks, a level that corresponds to natural hearing that typically does not require cochlear implantation. Seventy percent demonstrated an auditory brainstem response at 90 decibels or below, an objective electrophysiological confirmation of hearing function. Among those followed to 48 weeks, all prior responders maintained their response, and 42 percent achieved normal hearing that included the ability to detect whispers. These are not modest improvements. They are the kind of results that change what physicians tell families at the moment of diagnosis.
The Free Pricing Decision and What It Signals
Regeneron's announcement that Otarmeni will be provided at no cost to clinically eligible patients in the United States is the kind of decision that demands careful interpretation. Gene therapies for rare diseases have historically commanded prices in the hundreds of thousands or even millions of dollars, justified by the argument that a one-time curative treatment replaces years of ongoing care costs. Regeneron has inverted that logic entirely.
The company's chief scientific officer George Yancopoulos framed the decision as a statement about what the biopharmaceutical industry can be. That framing is worth taking seriously. Otarmeni targets an ultra-rare condition affecting approximately 50 newborns per year in the United States. The commercial revenue potential was always limited. But the decision to make the therapy free is not simply a concession to small market size. It is a deliberate positioning of Regeneron as a company that views its genetic medicine platform as a scientific and reputational asset, not merely a commercial one.
The timing is also notable. Regeneron announced the Otarmeni approval on the same day it unveiled a Most Favored Nation drug pricing agreement with the White House, becoming the last of 17 major drugmakers targeted by the Trump administration to sign on to the MFN framework. The juxtaposition of a free gene therapy and a pricing accord with the administration is not accidental. It is a carefully constructed narrative about a company that takes drug access seriously, at a moment when the political environment around pharmaceutical pricing has never been more charged.
A New Regulatory Pathway Makes Its Debut
Otarmeni carries another distinction beyond its clinical and commercial novelty. It is the first gene therapy approved under the FDA's Commissioner's National Priority Voucher program, a regulatory mechanism introduced under the current administration to accelerate review of treatments for serious conditions. The program, which grants priority review vouchers to drugs with Breakthrough Therapy designations in certain categories, has been controversial since its introduction, with some lawmakers and researchers questioning whether it adequately balances speed with rigor.
The Otarmeni approval will inevitably become a reference point in that debate. The drug received accelerated approval, meaning continued approval is contingent on verification of clinical benefit in the confirmatory portion of the CHORD trial. That is a standard condition for accelerated approval, and it is appropriate given the relatively small trial size. But the fact that the first gene therapy approved under the CNPV program is for a condition affecting 50 newborns per year, with compelling clinical data and a free pricing model, gives the program a favorable early case study. Whether that translates into broader confidence in the pathway will depend on how subsequent approvals under the program are handled.
The Platform Story Behind the Drug
Regeneron acquired the technology underlying Otarmeni through its 2023 purchase of Decibel Therapeutics for $109 million. That acquisition, modest by the standards of recent biopharma deal-making, has now produced the company's first approved genetic medicine and the first gene therapy for OTOF-related hearing loss in history. The return on that investment, measured in scientific and reputational terms, is already substantial.
More important than the single approval is what it represents for Regeneron's broader genetic medicine ambitions. The company has been building its genetic medicine platform for eight years, spanning gene therapy, gene editing, and RNA-based gene silencing. Otarmeni is the first clinical expression of that platform to reach approval, but it is not the last. Regeneron is already investigating genetic approaches to acquired and age-related hearing loss, conditions that affect millions rather than dozens of patients annually. The otoferlin story has demonstrated that the company can take a gene therapy from concept to approval with scientific rigor and commercial discipline. That proof of execution matters enormously as the platform matures.
What This Means for the Field
The approval of Otarmeni arrives at a moment when gene therapy is navigating a complicated period. Several high-profile programs have encountered regulatory setbacks, manufacturing challenges, or safety concerns that have tempered the field's earlier optimism. The CHORD trial data, with its clean safety profile and durable efficacy signals, provide a counterpoint to that narrative. A gene therapy that works, that is well-tolerated, and that can be delivered through a surgical approach already familiar to the clinical community is a different proposition from the more complex systemic gene therapies that have struggled.
For the families of children born with OTOF-related hearing loss, the approval is the end of a long wait and the beginning of a new chapter. For the broader field of genetic medicine, it is a demonstration that the promise of gene therapy, the idea that a single intervention can correct a genetic defect and restore normal function, is not merely theoretical. It is now, for at least one condition, a clinical reality. The question the field will be asking in the months ahead is which condition comes next.